“The virus acts like no pathogen humanity has ever seen.”
I read this quote in a recent article entitled, “How does coronavirus kill? Clinicians trace a ferocious rampage through the body, from brain to toes,” published in Science Magazine on April 17, 20201. To summarize the article, COVID-19 attacks almost anything in the body, and doctors are struggling to understand the full damage; this is because doctors are still catching up on understanding the symptoms of COVID-19. They are only now piecing together the symptoms patients didn’t realize had been COVID-19 related or didn’t have the words to describe what was happening to their bodies.
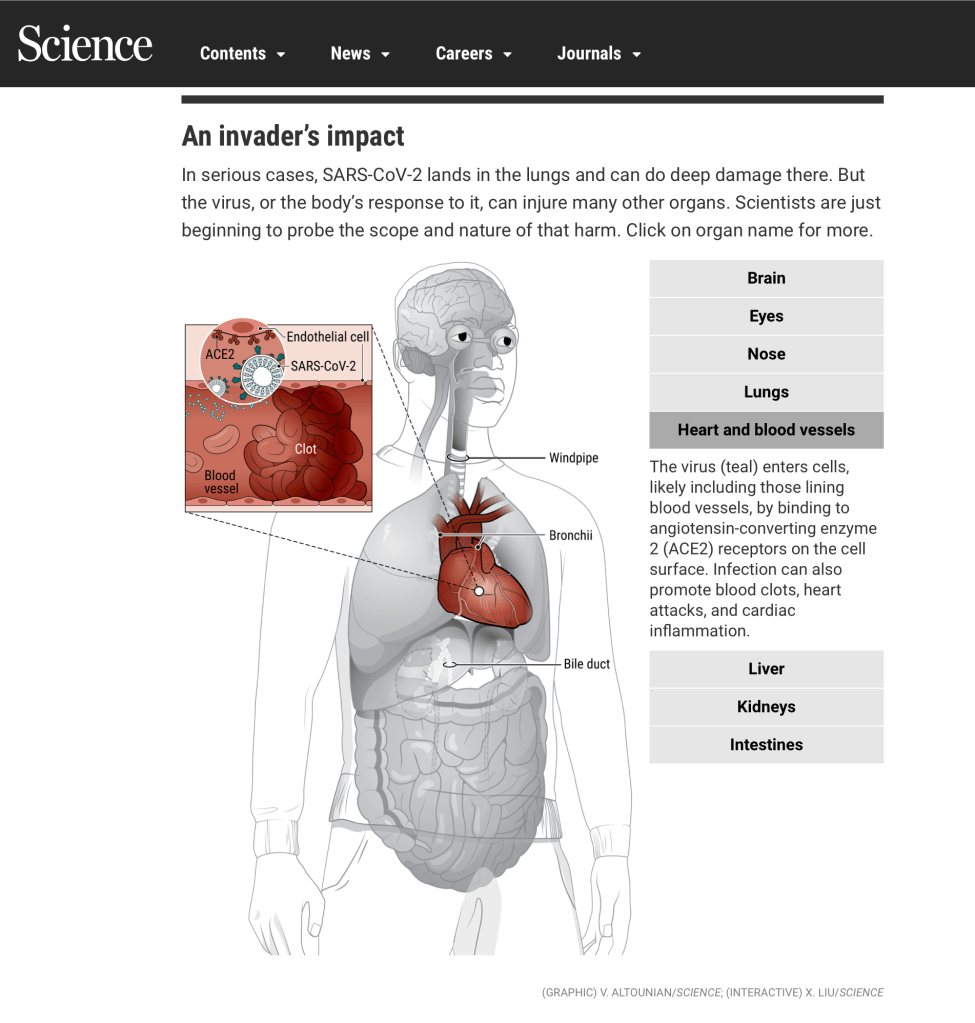
This article describes what I and many others, “seemingly mild” COVID-19 infected patients have been experiencing. Contrary to what doctors once thought, damage, inflammation, and infections are happening systematically across our bodies as a result of COVID-19, well beyond the confines of the lungs.
Which makes me wonder: how many people are experiencing these COVID19 symptoms that go incorrectly diagnosed or untreated because they cannot accurately and persistently communicate with their treating physician?
I was recently in the COVID-19 emergency department due to new symptoms after having COVID-19 but no longer testing positive. I explained to the on-call doctor that I had severe pain in my liver, kidneys, and lower abdomen. She looked at me and said, “so you have pain in your stomach?” They gave me antacids.
As I expected, the pain didn’t subside or go away. I repeated myself and told the on-call doctor that I knew where my anatomy was and that the pain I felt was different than “stomach pains.” I pushed her and the rest of the medical care team to run tests. I was immediately referred to a specialist when the test results came back.2
I share this story because I often hear from friends, and now readers of my blog, how difficult it is to communicate with their healthcare providers in a way that brings results.
My current PCP at Stanford is a great partner in advocating for my health. I know she is invested in my welfare and works with me to improve my quality of life. I’ve also moved around a lot in my career, and with insurance tied to an employer, having a fantastic doctor has not always been the experience.
I know that you may currently feel that you do not have the best partnership with your doctor. Or maybe you don’t have a current doctor, or you lack health insurance and aren’t sure how to navigate a conversation with a healthcare team you don’t know.
I’ve read so many messages from readers that have had the opposite experience from my own. Readers shared that they have often felt unheard by their medical care team, their symptoms dismissed, and, at times, they were sent home without being treated. Readers repeatedly asked me for tips on how to “get better help.”
So here are my top five tips on how to advocate for yourself, especially during a crisis. It could save your life.
1. Document Your Symptoms
One of the most critical tools in advocating for your healthcare is keeping a rolling list documenting the date and times of all of the symptoms you experience. Doctors treat their patients based on known symptoms and how these symptoms progress. Try to be precise in how you describe your symptoms. Was the pain throbbing, stabbing, or aching? Does it come and go, or is it always there? Do you feel it more while doing an activity or at a specific time in the day?
2. Use the correct names when you can.
I was able to advocate for myself by using the correct anatomical names with my healthcare team. I know this ability comes from growing up with a parent in the medical field who modeled this behavior. I’m also aware that pre-med courses in college have enabled me with additional knowledge. However, there are FANTASTIC resources online to help anyone learn correct anatomical names.
A quick google search for “games to help learn anatomy” will bring up a few game-like websites geared toward learning the human body. Some of the sites can are for grade-school kids; others, like Real Body Works (one of my favorites), are a bit more advanced.
This tip also applies to managing mental healthcare and treatment. In order to best advocate for yourself, especially for symptoms that can’t always be seen visibly by your healthcare provider. Using correct terms like CBT, DBT, activities of daily life, anxiety vs depression, fatigue vs lack of desire, and knowing your proper medication names will help ensure better diagnosis and continued treatment by your healthcare team.
3. Ask questions. LOTS of questions.
Have you ever heard of the adage, “There are no stupid questions?” Well, that is certainly true when it comes to your health and welfare. Ask a lot of questions, and if you don’t understand the answer, ask your healthcare provider to explain it another way. Keep asking questions until you feel comfortable enough to tell in your own words what is going on with your health. I take out my phone’s notepad app and take down notes. Having notes from the doctor’s talking points recorded in my phone also helps me ask better follow up questions.
4. Use the process of elimination
If you’ve ever watched House, M.D., this concept will be very familiar to you. Each episode of House, M.D., the doctor, played by Hugh Laurie and his team of specialists, would try to figure out the most allusive medical cases through the process of elimination. This process is accurate in real-life.
Doctors treat the symptoms and then observe what happens to determine the next course of action: either the treatment worked, or they need more information. Doctors gather more information to understand better what is causing your symptoms by trying another approach to treatment, running more tests and labs, or by doing all simultaneously.
You can better advocate for yourself by understanding that this process determines what your healthcare team will choose to do next. Approach your doctor with deductive reasoning and logic to provoke them to take a closer look. This step is also where your notes from Tips #1 and #3 will come in handy.
In my example above, I reminded the on-call doctor that the treatment of antacids did not help or change my symptoms. I told her that I was still experiencing pain and asked her, “What is the next course of treatment?”
Which leads me to tip 5:
5. Be persistent.
You know your body better than anyone else, and no one will stick up for you as well as you can. Being persistent is especially pertinent if you are a woman or a person of color, as studies have shown there is inherent pain bias, especially toward women.
Biases about women and pain lead to disparities in treatment. There are numerous articles on how women who enter into an ER experiencing life-threatening symptoms are often sent home by their doctors. In contrast, ER doctors will immediately treat men exhibiting the same symptoms.
Advocating for yourself means being persistent and not talking yourself out of insisting that your healthcare team continues to either “treat your symptoms until something works” and insist on “additional tests to rule out potential causes.”
Don’t be passive but be direct and assume treatment. I intentionally don’t use phrases like “will you run more tests?” I say, “What are your next steps to treat my symptoms?” “What tests will you now run to rule out other possible causes?”
6. BONUS TIP: Keep up to date with reputable sources
I cannot stress enough how important it is only to get your healthcare information from reliable, authoritative sources; this is especially important with COVID19 related issues. It’s one of the reasons I include links and quote my references in my blog.
The most authoritative subject matter experts are continually publishing new findings on the World Health Organization website. There are two sections of the WHO site: one for the general public and one for healthcare workers and scientists. The part of the WHO website for healthcare professionals and scientists has a page for White Papers to be published after they have been peer-reviewed–e.g., determined by the medical community to be accurate and authoritative. Once these white papers “go viral” within the medical community and are found to be shared globally, the findings get posted in simple, everyday language on the public side of the WHO website. Information about COVID-19 symptoms and recovery on the WHO’s site has consistently been 1-2 months ahead of the media.
Additional resources I recommend that cover both COVID19 and other health issues that you can use when researching are:
1. Stanford Health

2. Harvard Health
3. Mayo Clinic
4. World Health Organization
Other References:
2 https://rebeccakelly.blog/2020/04/15/3-things-you-need-to-know-now-about-recovering-from-covid19/

Leave a comment